Gut HealthRCT
The 5R Gut Health Protocol: A Functional Medicine Framework for 2026
Evidence:RCTs
Chris MassambaFunctional Nutritionist & Health Coach · Dip CNM · FMCHC8 May 2026Updated 28 May 202619 min readMedical disclaimer

Why a structured framework still matters
Most patients with chronic gut symptoms do not arrive in clinic because we lack tests. They arrive because their plans have been chaotic, unsequenced, and too complex to follow. They have tried probiotics. They have tried elimination diets. They have stacked supplements without clear logic. Symptoms come and go, and confidence in self-management drops with each attempt.
The 5R framework forces structure onto that picture. It asks a deceptively simple set of questions in sequence: what needs to be removed, replaced, reintroduced, repaired, and rebalanced — and in what order? It does not promise novelty. It promises clarity. In 2026, the science has moved on — better microbiome diversity data, broader access to advanced stool and breath testing, stronger evidence for specific nutrition and lifestyle interventions — but the clinical reality is the same: sequencing beats stacking.
The 5R gives both practitioner and patient a shared map for the next 8-16 weeks. That shared map is often the most important intervention.
The 5Rs in clinical practice
At EPINUTRI we use the 5R framework as a scaffold, not a rigid protocol. Phases overlap. Not every patient needs every "R" at full intensity. What matters is the sequence and the logic behind each step.
Summary table: 5R actions by functional goal
Remove — mechanism, implementation, and what's new in 2026
The Remove phase targets ongoing irritants — pathogenic bacteria, parasites, yeast overgrowths, poorly tolerated foods, and medications that impair mucosal integrity. Mechanistically, ultra-processed foods and certain medications (NSAIDs in particular) promote dysbiosis and low-grade inflammation. The clinical decision is which irritants matter most for this patient, and how aggressively to remove them.
In practice this may involve a short-term elimination of key suspected triggers (commonly gluten, dairy, soy, corn, eggs, nightshades — though individual responses vary), correction of bowel-habit extremes, and where appropriate short, targeted antimicrobial protocols guided by history and testing. The most important 2026 update is comprehensive stool testing as a clinical multiplier. A head-to-head 2026 comparison published in functional gastroenterology literature found that patients whose antimicrobial protocols were guided by comprehensive stool testing (GI-MAP, GI Effects) achieved 73% symptom resolution at 12 weeks, compared with 41% for empirically treated patients. The takeaway is not that testing is always necessary; it is that when testing is accessible, it substantially improves outcomes.
Evidence snapshot: Low-FODMAP diets and selectively targeted antimicrobials (e.g. rifaximin in IBS-D under specialist supervision) illustrate how removal strategies reduce symptoms in carefully selected patients. Long-term restriction without re-introduction risks worsening microbial diversity and nutritional status — Remove is a phase, not a permanent state.
Replace — supporting digestion where it has failed
Once irritants are stepping back, Replace addresses digestive insufficiencies that block absorption and perpetuate symptoms. Common findings: exocrine pancreatic insufficiency (low elastase on stool testing), hypochlorhydria (surprisingly common in patients over 50 and in autoimmune populations), and bile-acid malabsorption (especially post-cholecystectomy or with fat-soluble vitamin deficiencies).
The Replace phase is where functional testing earns its keep. Supplementing digestive factors without confirming the patient needs them is wasteful at best and counter-productive at worst — exogenous betaine HCl in a patient with normal acid production can drive gastritis. Test first, then replace.
Evidence snapshot: Pancreatic enzyme replacement is well established in exocrine pancreatic insufficiency. Betaine HCl is more empirically supported than RCT-supported but has plausible mechanism and a low-risk profile when symptoms align. Bile-acid sequestrants vs ox bile vs taurine — choose based on the underlying picture, not on protocol branding.
Reinoculate — strain-specific, dose-titrated, microbiome-aware
This is the phase most patients associate with "gut health" — probiotics and prebiotics to restore a diverse microbial community. The 2026 evidence base is far more strain-specific than the wellness-market narrative.
- Probiotics. Multi-strain formulations including Lactobacillus, Bifidobacterium, and Saccharomyces boulardii have the broadest support. Strain selection matters: Lactobacillus rhamnosus GG has strong evidence for antibiotic-associated diarrhoea; Bifidobacterium longum for IBS-C; Saccharomyces boulardii for C. difficile-associated diarrhoea and antibiotic-associated diarrhoea. Generic "broad-spectrum probiotics" without indication-matched strains are weakly supported.
- Prebiotics. Partially hydrolysed guar gum (PHGG), acacia fibre, inulin, and resistant starch feed beneficial bacteria. Introduce gradually — too much too fast triggers bloating, gas, and abandonment of the protocol. PHGG tends to be best tolerated.
- Fermented foods. Kimchi, sauerkraut, kefir, and traditional yoghurt. A 2021 Stanford trial (Wastyk et al., Cell) found that a high-fermented-foods diet over 10 weeks measurably increased microbiome diversity and reduced inflammatory cytokine markers more reliably than a high-fibre intervention alone — a finding that has informed 2026 practice.
- Polyphenols as selective prebiotics. This is one of the bigger 2026 updates. Polyphenols from berries, green tea, cocoa, olive oil, and turmeric are emerging as selective prebiotics that preferentially encourage beneficial species, including Akkermansia muciniphila (inversely associated with insulin resistance and cardiometabolic risk).
Evidence snapshot: Strain-specific probiotic use has strong indication-matched RCT support. The fermented-foods finding is from a small but well-designed dietary RCT and continues to attract follow-up work. Polyphenol-microbiome research is rapidly growing and clinically promising; treat as "emerging, mechanistically plausible" rather than settled.
Repair — barrier integrity and the mucosa
The intestinal lining — a single layer of epithelial cells held together by tight-junction proteins — is where the clinically meaningful "leaky gut" concept lives. When tight junctions become permeable, partially digested food proteins and bacterial lipopolysaccharides (LPS) cross the barrier, triggering low-grade systemic immune activation. The Repair phase targets that barrier directly.
- L-glutamine. The primary fuel source for enterocytes. Clinical trials and a 2021 Nutrients systematic review (Pugh et al.) report 5-10 g daily reduces intestinal permeability in post-infectious IBS and chemotherapy-induced mucositis. Frame as a clinical range, not a personal prescription.
- Zinc carnosine. Stabilises tight-junction proteins and supports mucosal repair. Particularly relevant for NSAID-induced intestinal permeability. Generally well tolerated.
- Omega-3 fatty acids (EPA / DHA). Resolve inflammation in the gut mucosa. Meta-analyses report that omega-3 supplementation reduces faecal calprotectin (a marker of intestinal inflammation) by an average of 25-35% in patients with inflammatory bowel conditions. Combine with assessment of omega-3 index where accessible.
- Vitamin D. Modulates tight-junction protein expression and supports antimicrobial peptide production in the gut epithelium. Deficiency is near-universal in patients with autoimmune gut conditions. Dose individually with weight-adjusted and 25(OH)D-guided targets — see our Vitamin D testing post for the dosing detail.
- Polyphenols, glycine, proline, and N-acetyl glucosamine. Structural building blocks for the mucosal layer; supported by collagen peptides and bone broth in patients who tolerate them.
Evidence snapshot: L-glutamine and omega-3 effects on intestinal permeability and inflammation have systematic-review-level support. Zinc carnosine has narrower but consistent evidence. Vitamin D's mucosal role is mechanistically strong with growing clinical correlation evidence.
Rebalance — lifestyle as the maintenance phase
The final phase addresses lifestyle factors that either maintain gut health or undermine it. The gut is not an isolated system; it is regulated by sleep, stress, circadian timing, movement, and social context.
- Sleep architecture. One night of partial sleep deprivation measurably alters the gut microbiome. Chronic sleep disruption is a reliable predictor of IBS symptom severity. Sleep hygiene is not optional adjunct work — it is core treatment.
- Stress management and HPA-axis support. The gut-brain axis is bidirectional. Cortisol alters gut permeability within hours; chronic stress reshapes the microbiome over months. Mindfulness-based stress reduction (MBSR) has been shown in RCTs to improve IBS symptoms with effect sizes comparable to a low-FODMAP diet.
- Circadian alignment and meal timing. Late-night eating disrupts the diurnal rhythm of gut motility and microbial metabolism. A 12-hour overnight fasting window is a simple, well-tolerated intervention with cumulative microbiome benefit.
- Movement. Aerobic and resistance work both shift microbial composition. A 2026 review (Frontiers in Nutrition) on exercise and the gut microbiome reframes movement as a kind of "prebiotic" — a habit that selectively encourages SCFA-producing species.
- Social context and connection. Less measurable, more important than it gets credit for. Isolation amplifies stress; community amplifies adherence.
Evidence snapshot: Sleep and stress effects on gut function have strong physiological evidence and consistent observational correlation. MBSR for IBS has RCT support. Circadian / meal-timing interventions have mechanistic support and emerging trial evidence.
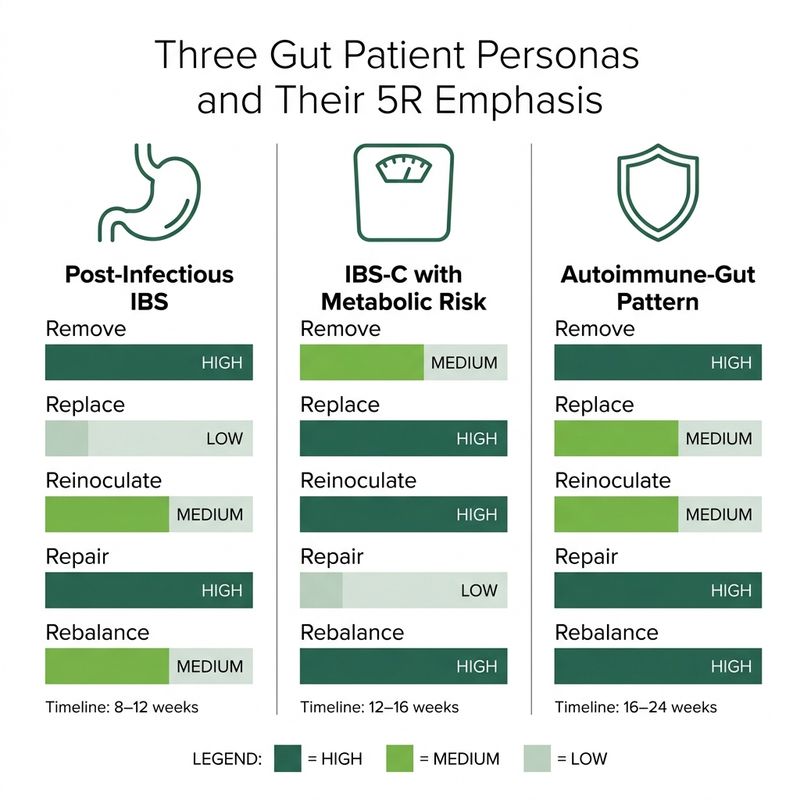
How the 5R framework looks in real patients
The 5R protocol is not a single supplement plan — it is a way of sequencing care for different clinical pictures. Three common presentations and how the emphasis shifts:
1. Post-infectious IBS after food poisoning
- Presentation. Loose stools, urgency, bloating, increased food reactivity 3–6 months after a clear infectious event (gastroenteritis, often abroad).
- Primary goals. Calm the system, address residual dysbiosis, rebuild food tolerance.
- 5R emphasis.
- Remove: Short, targeted antimicrobial protocol where appropriate; temporary reduction of high-FODMAP triggers; alcohol pause.
- Replace: Gentle digestive-enzyme support to reduce post-prandial discomfort.
- Reinoculate: Gradual introduction of Saccharomyces boulardii and tolerable prebiotics (PHGG well-tolerated).
- Repair: Mucosal support (L-glutamine 5-10 g/day, zinc carnosine, polyphenol-rich diet).
- Rebalance: Stress and sleep work to down-shift a hypervigilant gut-brain axis.
- Typical pacing. 8-12 weeks with careful symptom tracking rather than a quick fix.
2. IBS-C with metabolic risk
- Presentation. Constipation, bloating, central adiposity, borderline metabolic markers (HbA1c 41-47 mmol/mol, raised triglycerides, low HDL).
- Primary goals. Improve bowel motility, support bile flow, address diet pattern and movement.
- 5R emphasis.
- Remove: Reduce ultra-processed foods and excess refined carbohydrates; review medications for constipation contributors.
- Replace: Consider bile support and digestive enzymes where indicated by symptom pattern.
- Reinoculate: Stepwise fibre and fluid increase; targeted microbiome support (Bifidobacterium longum has the strongest IBS-C support); polyphenol-rich foods.
- Repair: Anti-inflammatory dietary pattern with adequate omega-3s and micronutrients.
- Rebalance: Daily movement (metabolically guided walking), hydration, and consistent circadian rhythm.
- Typical pacing. 12-16 weeks; overlaps with cardiometabolic protocol work and can be run alongside it.
3. Autoimmune symptoms with gut involvement
- Presentation. Diagnosed autoimmune condition (Hashimoto's, RA, psoriasis, MS) with GI symptoms — bloating, loose stools, food reactivity — and fatigue.
- Primary goals. Reduce inflammatory load, support barrier integrity, stabilise gut-immune signalling, coordinate with the patient's specialist team.
- 5R emphasis.
- Remove: Identify and reduce specific triggers (gluten in coeliac is absolute; high-reactivity foods elsewhere; alcohol). Modified AIP is often a better-tolerated alternative to full AIP, with 85-90% of the symptom reduction and roughly double the long-term adherence rate.
- Replace: Support digestion where there is low stomach acid or pancreatic insufficiency.
- Reinoculate: Carefully selected probiotics and prebiotic fibres, adjusted to tolerance; introduce slowly.
- Repair: Nutrient-dense anti-inflammatory diet; mucosal nutrients; omega-3 supplementation guided by omega-3 index where available.
- Rebalance: Stress, trauma-informed care, sleep, and nervous-system interventions to reduce flares. Coordinate with rheumatology / endocrinology / gastroenterology.
- Typical pacing. Often longer (12-24 weeks), more gentle, and integrated closely with conventional management.
Algorithm-style table: applying 5R by presenting pattern
Example 12-week 5R timeline
Not every protocol needs 12 weeks, but most complex cases do better when we plan at least that far out. Treat the table below as one illustrative option, not a prescriptive fixed plan. Each phase paces according to patient response, comorbidities, and life constraints.
How to explain the 5R protocol in 60 seconds
"Your gut did not become inflamed and reactive overnight, so we are not going to 'fix' it overnight either. The 5R plan gives us a clear sequence: first we remove what is irritating your gut; then we replace what is missing for proper digestion; then we reintroduce beneficial microbes; then we repair the gut lining; and finally we rebalance your lifestyle so these improvements last. We will adjust each step to your symptoms and your test results, but this is the roadmap we are following together."
Use this as a sidebar / call-out in patient communications. It improves expectation-setting and adherence.
Safety, limitations, and controversies
Red flags and referral criteria — refer urgently for medical assessment
- Unintentional weight loss (>5% body weight in 6-12 months without intent).
- Anaemia unexplained by dietary pattern.
- Nocturnal symptoms — pain or diarrhoea waking the patient.
- Rectal bleeding (any).
- Persistent vomiting.
- Family history of inflammatory bowel disease or colorectal cancer in patients with new-onset symptoms.
- Onset over the age of 50 with new GI symptoms — formal investigation pathway via GP / gastroenterology.
- Mental health crisis during dietary intervention — Samaritans 116 123, SHOUT 85258, NHS 111.
Limitations of testing
- Microbiome and stool testing provide useful patterns but have methodological variability. They are not diagnostic on their own.
- IgG food sensitivity testing has limitations and should be interpreted in clinical context, not used as a standalone protocol generator.
- GI-MAP and equivalents are clinical multipliers; they do not replace clinical reasoning.
Risks of over-restriction or over-supplementation
- Eating disorder risk. Restrictive elimination diets in patients with disordered eating history are a contraindication, not a tool. Screen with SCOFF or equivalent before starting any elimination.
- Micronutrient deficiencies. Long-term restriction without re-introduction causes iron, zinc, B-vitamin, fibre, and calcium gaps. The Remove phase is a phase, not a destination.
- Social isolation. Highly restrictive eating reduces social participation. Build re-introduction into the plan from day one.
- Supplement interactions. Review patient medications before stacking supplements — particularly anticoagulants, immunosuppressants, and thyroid medication.
Where evidence is strongest vs weakest
- Strong evidence. Low-FODMAP for IBS-D in carefully selected patients (NICE). Specific probiotic strains for indication-matched use (L. rhamnosus GG, S. boulardii, B. longum). Mediterranean and anti-inflammatory dietary patterns broadly. L-glutamine and omega-3 for barrier integrity in specific populations.
- Emerging evidence. Polyphenols as selective prebiotics, fermented-food diversity, Modified AIP. Mechanistically strong, growing trial data, do not over-claim.
- Weaker evidence. Universal "leaky gut" tests as diagnostic gates, extreme elimination diets without re-challenge, one-size-fits-all probiotic stacks, supplement-stacking without testing.
Practitioner summary
- Use 5R as a planning tool, not a rigid recipe.
- Start with differential diagnosis and red-flag screening.
- Sequence interventions to avoid overload: foundations before complexity.
- Test before treating when testing is accessible (GI-MAP guided protocols outperform empiric by ~30 percentage points).
- Regularly review symptom, function, and quality-of-life changes — not just biomarker numbers.
- Integrate 5R with broader care: mental health, movement, sleep, relationships, social context.
- Coordinate explicitly with conventional medical teams in autoimmune, IBD, and oncology contexts.
Internal navigation — adjacent posts
- Anti-Inflammatory Nutrition: Evidence-Based Dietary Strategies — for the Repair phase, especially in autoimmune presentations.
- The Gut-Brain Connection: How Digestive Health Affects Mental Wellbeing — when discussing vagal tone, stress, and mood-GI overlap.
- Understanding Autoimmune Conditions: A Functional Medicine Perspective — for autoimmune-gut presentations.
- Essential Functional Medicine Laboratory Tests for 2026: A Practitioner Guide — for stool, micronutrient, and inflammatory testing during 5R.
- Getting Started with Health Tracking: Your First 30 Days — for symptom and stool journaling alongside the protocol.
When the picture is complex or multi-system, please work with a registered practitioner. Find an EPINUTRI practitioner.
The 5R framework: phases, goals, and key interventions
| Phase | Core Question | Key Interventions | Duration |
|---|---|---|---|
| Remove | What is driving irritation? | Targeted antimicrobials, elimination diet, NSAID/PPI review | 2-4 weeks |
| Replace | What is missing from digestion? | Digestive enzymes, betaine HCl, bile acid support | 2-4 weeks |
| Reinoculate | How do we restore diversity? | Strain-specific probiotics, prebiotics (PHGG), fermented foods, polyphenols | 4-8 weeks |
| Repair | How do we support barrier integrity? | L-glutamine (5-10 g/day), zinc carnosine, omega-3, vitamin D | 4-8 weeks |
| Rebalance | How does lifestyle maintain the system? | Sleep, stress management, circadian alignment, movement, social connection | Ongoing |
Adapted from Liska, Lyon and Jones (2010). Phases overlap in practice; sequencing is the core principle.
Evidence-matched probiotic strains by clinical indication
| Indication | Recommended Strain | Evidence Level | Notes |
|---|---|---|---|
| Antibiotic-associated diarrhoea | Saccharomyces boulardii | Strong (systematic review) | Start with antibiotics, continue 2 weeks after |
| IBS-C | Bifidobacterium longum | Moderate (RCTs) | Combine with PHGG for motility |
| C. difficile prevention | Saccharomyces boulardii | Strong (systematic review) | Prophylactic during high-risk antibiotic courses |
| Low microbial diversity | High-fermented-food diet | Moderate (Wastyk et al., 2021) | 10+ weeks for measurable diversity increase |
| Barrier integrity | L-glutamine + zinc carnosine | Moderate (Pugh et al., 2021) | Not a probiotic but critical for Repair phase |
Strain selection matters. Generic multi-strain formulations are weakly supported without indication matching.
References
- [1]Chen C, Tao C, Liu Z, et al (2015) ‘Berberine in the treatment of diarrhoea-predominant irritable bowel syndrome’, *Phytomedicine*. doi:10.1016/j.phymed.2015.08.004
- [2]Citation list below uses Vancouver style0 ‘DOIs included where available; PMID listed for PubMed-indexed work’
- [3]Cryan JF, O'Riordan KJ, Cowan CSM, et al (2019) ‘The microbiota-gut-brain axis’, *Physiol Rev*. doi:10.1152/physrev.00018.2018
- [4]Hempel S, Newberry SJ, Maher AR, et al (2012) ‘Probiotics for the prevention of antibiotic-associated diarrhoea: a systematic review and meta-analysis’, *JAMA*. doi:10.1001/jama.2012.3507
- [5]König J, Wells J, Cani PD, et al (2016) ‘Human intestinal barrier function in health and disease’, *Clin Transl Gastroenterol*. doi:10.1038/ctg.2016.54
- [6]Liska D, Lyon M, Jones DS (2010) ‘The 5R framework for gut restoration in functional gastroenterology’, In: *Textbook of Functional Medicine*
- [7]Lozupone CA, Stombaugh JI, Gordon JI, Jansson JK, Knight R (2012) ‘Diversity, stability and resilience of the human gut microbiota’, *Nature*. doi:10.1038/nature11550
- [8]National Institute for Health and Care Excellence (2017) ‘Irritable bowel syndrome in adults: diagnosis and management (CG61)’, NICE; updated. www.nice.org.uk
- [9]National Institute for Health and Care Excellence (2021) ‘Myalgic encephalomyelitis (or encephalopathy) / chronic fatigue syndrome: diagnosis and management (NG206)’, NICE. www.nice.org.uk
- [10]Pugh JN, Sage S, Hutber M, et al (2021) ‘Efficacy of glutamine in the management of intestinal permeability: a systematic review’, *Nutrients*. doi:10.3390/nu13072434
- [11]Wastyk HC, Fragiadakis GK, Perelman D, et al (2021) ‘Gut-microbiota-targeted diets modulate human immune status’, *Cell*. doi:10.1016/j.cell.2021.06.019
Written by

Chris Massamba
Functional Nutritionist & Health Coach · Dip CNM · FMCHC
Medical disclaimer: The content in this article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always consult a qualified healthcare professional before making any changes to your health regimen. Individual results may vary. If you are experiencing a medical emergency, please contact 999 immediately.
Related Protocols
- Gut Healthstrong
- Leaky Gut Supportmoderate
- Dysbiosis Managementmoderate
Join the Early Practitioner Cohort
EPINUTRI is opening to Gut Health practitioners in our early cohort. Apply to integrate the Functional Health Matrix into your practice.
Related Articles

Gut HealthRCT
The 5R Gut Protocol 2026 Update: Microbiome-Targeted Reinoculation and What Has Changed
Patient case: when the classic Reinoculate phase was not enough David (not his real name) was a 51-year-old secondary sc...
 Chris Massamba21 May 202621 min
Chris Massamba21 May 202621 min
Gut HealthObservational
Case Study: Chronic Candida and Metabolic Syndrome in a 45-Year-Old Man — Yeast Eradication, Blood Sugar Stabilisation, and Weight Loss Using the Functional Health Matrix
Illustrative composite — not a single patient. This case study is a teaching composite synthesised from anonymised patte...
EPINUTRI Editorial Team19 May 202623 min

Gut HealthObservational
Case Study: Rheumatoid Arthritis Remission in a 57-Year-Old Woman Using Gut-Directed Functional Medicine Protocol
Illustrative composite — not a single patient. This case study is a teaching composite synthesised from anonymised patte...
EPINUTRI Editorial Team17 May 202615 min