NutritionRCT
Essential Functional Medicine Laboratory Tests for 2026: A Practitioner Guide
Evidence:RCTs
Chris MassambaFunctional Nutritionist & Health Coach · Dip CNM · FMCHC8 May 2026Updated 28 May 202617 min readMedical disclaimer

Why advanced testing matters in 2026
Laboratory testing remains one of the most useful tools in functional medicine — but only when it answers a clear clinical question. The problem in 2026 is not a lack of available tests. It is the growing tendency to order broad, expensive panels without first defining what decision the result will change.
Practitioners now have access to more sophisticated testing than at any point in the discipline's history: standard biochemistry and hormone panels, advanced thyroid assessments, comprehensive stool analysis with PCR-based pathogen detection, micronutrient and organic acids profiling, cardiometabolic risk panels (CIMT, ApoB, fasting insulin, hs-CRP), and emerging mitochondrial-function diagnostics. Used well, these tools clarify mechanisms, stratify risk, and support more personalised interventions. Used poorly, they increase cost, confuse patients, and generate false certainty around weak or non-actionable findings.
A credible functional medicine approach to ordering always starts with three questions:
- What is the clinical hypothesis?
- Which test is most likely to change management?
- Does the result add value beyond history, examination, and foundational labs?
This mindset separates evidence-informed testing from expensive fishing expeditions — and it is the difference between a practitioner whose lab reasoning peers will reference, and one who hands every patient a bundle.
Principles for ordering labs responsibly
Before discussing specific panels, a few decision rules. These improve credibility because they signal restraint, not enthusiasm.
- Start with history, symptoms, medication review, and red-flag screening. A 20-minute history will out-perform a 20-marker panel for ~80% of presentations.
- Use foundational conventional labs before moving into advanced functional panels. Full blood count, U&E / CMP, LFTs, HbA1c, lipids, ferritin, B12, folate, vitamin D, CRP. These are inexpensive, widely standardised, and identify most of the common causes of chronic symptoms.
- Prioritise tests that are actionable, reproducible, and relevant to the presenting complaint. Reproducibility matters: some functional panels have inter-lab variability that limits clinical interpretation.
- Avoid ordering large bundles "just in case" when the pre-test probability is low. Bayesian common sense applies: ordering a low-yield test in a low-prevalence population produces more noise than signal.
- Re-test only when the result will meaningfully change treatment or prognosis. Retesting habits should be defined upfront, not adjusted to patient anxiety.
- Document rationale. Every order in the notes should have a sentence answering "what will I do differently based on this result?"
Which labs make sense for different clinical presentations
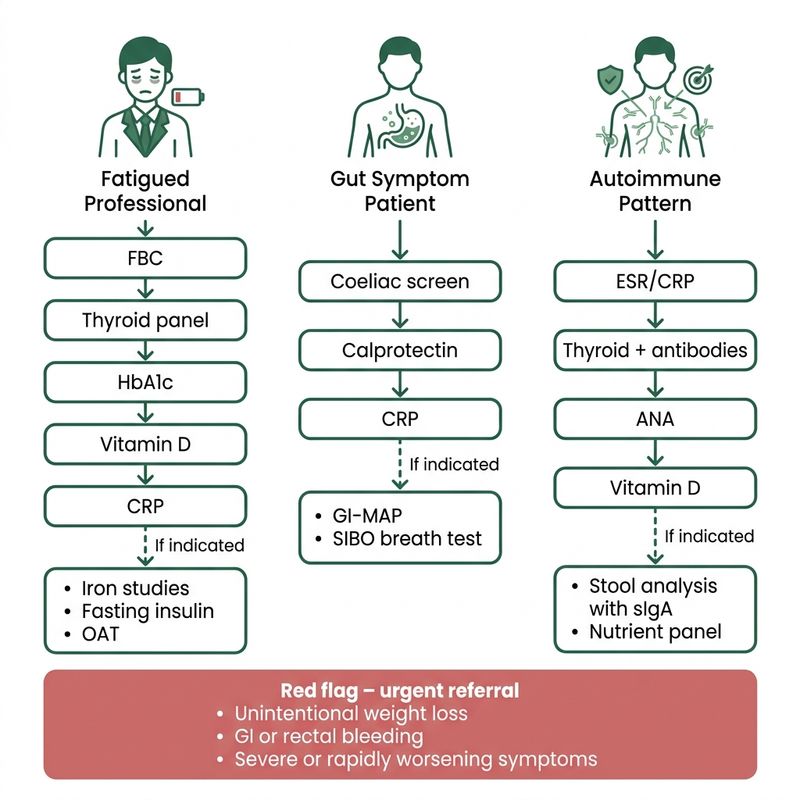
Lab selection should be guided by presentation, not by protocol branding. A fatigued executive, a patient with recurrent bloating, and someone with suspected autoimmunity may all benefit from testing, but the most useful starting points are not the same. Three common clinical pictures:
1. The fatigued high-performer
- Presentation. Persistent fatigue despite acceptable sleep, poor exercise recovery, brain fog, irregular meals, high stress load. Common in busy professionals 35–55.
- First-line labs. FBC, ferritin, B12 / folate, full thyroid panel (TSH + free T4 + free T3 + TPO antibodies), HbA1c, fasting glucose, vitamin D (25(OH)D), CRP, U&E / CMP, LFTs.
- Second-line considerations. Iron studies (transferrin saturation, soluble transferrin receptor), fasting insulin, morning cortisol context (if a strong HPA-axis story emerges), selected micronutrients where diet or absorption is plausibly compromised, omega-3 index.
- Clinical rationale. Fatigue is common, the differential is broad, and foundational screens commonly identify anaemia, iron insufficiency, thyroid dysfunction, dysglycaemia, or inflammatory burden — all treatable, none requiring expensive functional panels to detect.
2. The gut-symptom patient
- Presentation. Bloating, altered bowel habit (loose / hard / alternating), food reactivity, abdominal discomfort, incomplete response to dietary changes already attempted.
- First-line labs. FBC, CRP, coeliac screen (anti-TTG IgA + total IgA), ferritin, B12 / folate, U&E / CMP, stool calprotectin where IBD suspicion exists.
- Second-line considerations. Comprehensive stool analysis (GI-MAP or GI Effects), breath testing (lactulose / glucose for SIBO), pancreatic elastase, selected nutrient markers in chronic malabsorption patterns.
- Clinical rationale. The first clinical priority is distinguishing functional symptoms from inflammatory, infectious, or structural concerns. Until coeliac and IBD-pattern markers are clear, deep microbiome-focused interpretation can mislead the clinician about what is really driving symptoms.
3. The autoimmune-pattern patient
- Presentation. Multi-system symptoms, fatigue, joint pain, skin involvement, GI symptoms, fluctuating inflammatory signs. Often years of pre-diagnostic background before formal autoimmune diagnosis.
- First-line labs. ESR / CRP, FBC, U&E / CMP, full thyroid panel including TPO / TgAb antibodies, ANA or disease-specific immunology guided by presentation (rheumatoid factor / CCP, etc.), vitamin D, ferritin.
- Second-line considerations. Nutrient status (zinc, selenium, magnesium, omega-3 index), comprehensive stool analysis with secretory IgA, additional immune markers in collaboration with specialist care, fasting insulin in metabolic-overlap patients.
- Clinical rationale. Functional medicine adds value as an integrated layer, not as a substitute. Autoimmune work should remain grounded in proper medical diagnosis, referral pathways, and coordinated care with rheumatology / endocrinology / gastroenterology.
Table 1: Core vs advanced tests
Table 2: Lab ordering by clinical question
Common pitfalls in functional lab testing
The credibility of functional medicine does not improve when every patient leaves with twenty biomarkers and no clear interpretation strategy. It improves when practitioners use testing sparingly, document rationale clearly, and avoid turning weak associations into diagnoses.
Key pitfalls to avoid:
- Treating mildly abnormal markers as definitive pathology without correlating to symptoms, history, or repeat testing. A single borderline value almost never tells a complete story.
- Ordering advanced stool or micronutrient panels before basic medical screening is complete. Coeliac, IBD, hypothyroidism, and diabetes must be ruled out (or in) before deep functional interpretation makes sense.
- Repeating tests too frequently without a clinically meaningful reason. Microbiome and micronutrient profiles do not move in weeks, and chasing small numerical changes erodes patient confidence.
- Confusing optimisation targets with disease thresholds. "Optimal" ferritin (50-100 µg/L) is a functional preference, not a deficiency diagnosis at 30. Be explicit with patients about which kind of target you are using.
- Presenting speculative biomarkers as settled science. Where evidence is emerging, say so. The phrase "we are still learning about this marker" preserves clinical authority better than over-claiming.
- Test-driven rather than patient-driven planning. A 12-page lab report rarely improves a patient's day-to-day clinical management as much as a structured weekly tracking practice does.
A short paragraph acknowledging these limitations in any practitioner-facing article signals maturity and balance — exactly the signal that builds peer credibility.
A practical lab-ordering framework
The single most useful mental model for ordering is the lab-ordering pyramid:
- Base layer — history and examination. Always first. Cheap, fast, high-yield. A 20-minute timeline of symptoms, antibiotic history, dietary patterns, stress events, and prior treatments outperforms most panels.
- Second layer — foundational conventional labs. FBC, U&E / CMP, LFTs, HbA1c, lipids, ferritin, B12, folate, vitamin D, CRP. Add a full thyroid panel if symptoms warrant. This layer resolves the majority of presentations either by identifying a diagnosis or by clearly indicating which advanced panel is justified next.
- Third layer — targeted advanced functional panels. Comprehensive stool analysis, advanced thyroid (with antibodies and reverse T3 where indicated), CIMT in metabolic risk, organic acids in unexplained fatigue, fasting insulin / ApoB in cardiometabolic stratification. One panel at a time, with a clinical question.
- Top layer — repeat testing and monitoring. Only on a defined cadence (typically 8-12 weeks post-intervention for biomarkers that respond on that timescale; 12 months for stable markers like CIMT). Document the retesting rationale before ordering.
This pyramid is what a peer would recognise as defensible clinical reasoning — not a 15-test bundle ordered on the first consultation.
Safety, limitations, and when to refer
Functional testing complements but does not replace conventional pathways. Refer urgently for medical assessment if any of the following emerge during workup:
- Unintentional weight loss (>5% body weight in 6-12 months).
- Persistent vomiting, nocturnal symptoms, or rectal bleeding (any amount).
- Anaemia unexplained by dietary pattern.
- Severe joint swelling, organ-specific neurological signs, or unexplained acute fatigue with weight loss — investigate for inflammatory, autoimmune, or oncological causes via specialist pathway.
- Suspected eating disorder — refer to specialist services; restrictive functional protocols are contraindicated.
- Mental health crisis — Samaritans 116 123, SHOUT 85258, NHS 111 (urgent non-emergency), 999 (emergency).
Where evidence is strongest vs weakest, in the testing landscape:
- Strong evidence. Coeliac screening (anti-TTG IgA), TSH and antibodies for autoimmune thyroid, HbA1c for glycaemic status, lipid panel and ApoB for cardiovascular risk, ferritin for iron status, vitamin D 25(OH)D for repletion guidance.
- Emerging evidence. Comprehensive stool analysis with PCR pathogen detection (strong for indication-matched use, weaker as screening), advanced inflammatory markers (omega-3 index, hs-CRP optimisation targets), polyphenol-microbiome interaction biomarkers, dynamic mitochondrial-function panels.
- Weaker evidence. Universal "leaky gut" zonulin testing as a diagnostic gate, IgG food-sensitivity panels as standalone protocol generators, single-time-point cortisol as an HPA-axis snapshot.
Practitioner summary
- Order labs to answer a clinical question, not to find one.
- Start with history; finish with shared decision-making about what to do with the result.
- Use foundational conventional labs before advanced functional panels — always.
- Document rationale and retesting intent for every order.
- Resist the urge to over-explain mildly abnormal markers.
- Coordinate with conventional medical teams in autoimmune, IBD, oncology, and cardiovascular contexts.
- Treat lab reports as one input to a clinical decision, not as the decision itself.
How to explain functional testing in 60 seconds
"We have a wide range of tests available, but more testing is not always more useful. The plan we will follow is: first, your story and history — that often tells us most of what we need. Second, the standard blood tests your GP would order, because those are inexpensive, well-understood, and identify the most common causes of your symptoms. Only then, if those don't give us the answers, we look at specialised functional panels — and only the ones likely to change what we do for you. We are looking for the test that answers a specific question about your case, not a panel that gives us numbers we cannot act on."
Use this as a sidebar / call-out in patient communications. It improves expectation-setting and reduces the "more tests please" pressure that erodes both clinical reasoning and patient finances.
Internal navigation — adjacent posts
- The 5R Gut Health Protocol — when discussing GI-related test escalation and the testing-before-treating principle.
- Chronic Fatigue: Beyond Rest — when discussing fatigue workups, mitochondrial markers, and organic acids testing.
- Understanding Autoimmune Conditions — for inflammatory and antibody-based testing.
- Getting Started with Health Tracking — for symptom correlation, response tracking, and retesting rationale.
- Anti-Inflammatory Nutrition — when discussing CRP, omega-3 index, and inflammation-pattern markers.
When the picture is complex, multi-system, or beyond the scope of self-interpretation, please work with a registered practitioner. Find an EPINUTRI practitioner for coordinated care.
Lab-ordering pyramid: when to escalate from foundational to advanced testing
| Tier | What to Order | Cost | When to Use |
|---|---|---|---|
| 1: History + exam | 20-minute clinical timeline | Free | Always first. Resolves 80% of presentations. |
| 2: Foundational labs | FBC, U&E, LFTs, HbA1c, lipids, ferritin, B12, folate, vitamin D, CRP, thyroid panel | Low (NHS or ~£50-100 private) | Next step. Identifies anaemia, thyroid, dysglycaemia, inflammation. |
| 3: Targeted functional | Stool analysis (GI-MAP), OAT, CIMT, fasting insulin, ApoB, omega-3 index | Medium-High (£150-400 per panel) | Only when foundational is insufficient. One panel at a time. |
| 4: Repeat monitoring | Re-test at 8-12 weeks post-intervention (biomarkers); 12 months (stable markers) | Varies | Only with defined rationale documented upfront. |
Start at the base. Only escalate when the lower tier does not resolve the clinical question.
Evidence strength for functional testing modalities
| Evidence Tier | Test Examples | Clinical Confidence |
|---|---|---|
| Strong | Coeliac screen (anti-TTG IgA), TSH + antibodies, HbA1c, lipids + ApoB, ferritin, vitamin D 25(OH)D | High. Well-standardised, changes management reliably. |
| Emerging | Comprehensive stool analysis (PCR), hs-CRP optimisation, omega-3 index, dynamic mitochondrial panels | Moderate. Strong for indication-matched use; weaker as screening. |
| Weaker | Zonulin as leaky gut diagnostic, IgG food sensitivity panels, single-point cortisol | Low. High false-positive rate or limited clinical actionability. |
Guides practitioner credibility when discussing tests with patients and peers.
References
- [1]British Thyroid Association (2016) ‘Management of primary hypothyroidism: statement by the British Thyroid Association Executive Committee’, BTA. www.british-thyroid-association.org
- [2]Citation list below uses Vancouver style0 ‘DOIs included where available; PMID listed for PubMed-indexed work’, Specific paper-by-paper grading (Strong / Emerging / Expert opinion) is added when the post enters the schema-enforced clinical-references field
- [3]Ford ES, Greenlund KJ, Hong Y (2020) ‘ApoB, non-HDL cholesterol, and LDL cholesterol in predicting cardiovascular events: comparative review’, *J Am Coll Cardiol*
- [4]National Institute for Health and Care Excellence (2017) ‘Irritable bowel syndrome in adults: diagnosis and management (CG61)’, NICE; updated. www.nice.org.uk
- [5]National Institute for Health and Care Excellence (2015) ‘Coeliac disease: recognition, assessment and management (NG20)’, NICE. www.nice.org.uk
- [6]National Institute for Health and Care Excellence (2023) ‘Cardiovascular disease: risk assessment and reduction (CG181)’, NICE; updated. www.nice.org.uk
- [7]Patrick D, Aboud RA, Diabate F, et al (2024) ‘Organic acids testing in clinical practice: current evidence and limitations’, *Nutrients*
- [8]Pearce SHS, Brabant G, Duntas LH, et al (2013) ‘2013 ETA guideline: management of subclinical hypothyroidism’, *Eur Thyroid J*
- [9]Saberi-Karimian M, Tashakkori-Sabzevar F, Sahebkar A (2023) ‘Vitamin D measurement and supplementation: a state-of-the-art review’, *Eur J Clin Nutr*
- [10]Sridhar D, Wuttke DS, Sandborn WJ (2021) ‘Faecal calprotectin in inflammatory bowel disease: a clinical decision-support tool’, *J Crohns Colitis*
- [11]Wilson SR, Vahey GM, Ruge AS, et al (2024) ‘The clinical utility of stool testing in functional gastrointestinal disorders: a systematic review’, *Aliment Pharmacol Ther*
Written by

Chris Massamba
Functional Nutritionist & Health Coach · Dip CNM · FMCHC
Medical disclaimer: The content in this article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always consult a qualified healthcare professional before making any changes to your health regimen. Individual results may vary. If you are experiencing a medical emergency, please contact 999 immediately.
Related Protocols
- Gut Healthstrong
- Leaky Gut Supportmoderate
- Dysbiosis Managementmoderate
Join the Early Practitioner Cohort
EPINUTRI is opening to Nutrition practitioners in our early cohort. Apply to integrate the Functional Health Matrix into your practice.
Related Articles

NutritionExpert Opinion
Late-Spring Micronutrient Reset: Vitamin D Dosing After Winter — Why One Size Does Not Fit All
Why Late Spring Demands a Micronutrient Audit By mid-May, most of us in the United Kingdom have endured roughly six mont...
 Chris Massamba19 May 202612 min
Chris Massamba19 May 202612 min
NutritionSystematic Review
Dietary Guidance 2025-2030: What Functional Medicine Practitioners Need to Know
The Shifting Landscape of Dietary Guidance The 2025-2030 dietary guidelines represent a significant evolution in mainstr...
 Chris Massamba8 May 202610 min
Chris Massamba8 May 202610 min
NutritionExpert Opinion
New Dietary Guidance 2025-2030: Why Federal Recommendations Now Align with Functional Medicine
The Five Shifts That Matter 1. "Eat Real Food" Becomes Official Policy Previous dietary guidelines talked about nutrient...
 Chris Massamba8 May 20266 min
Chris Massamba8 May 20266 min